At Diabetes & Endocrine Treatment Specialists treating Gestational Diabetes is one of our top priorities. Treatment plans greatly improve pregnancy outcomes, for both mother and child. For many women, they’re able to achieve normal blood glucose levels through diet alone, however, some women may require medications.
We are here for you with 24/7 care 365 days a year.
What is Gestational Diabetes?
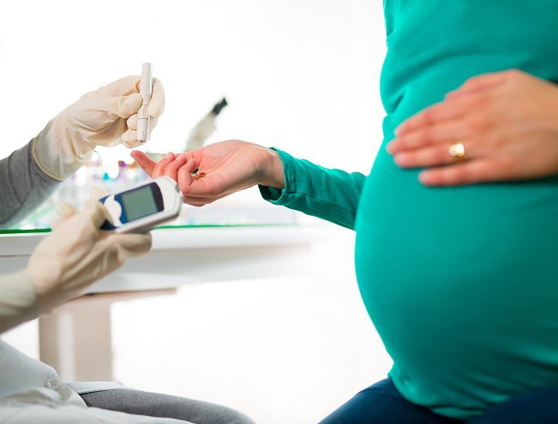
GESTATIONAL DIABETES EXPLAINED AS SIMPLY AS POSSIBLE…
GESTATIONAL DIABETES EXPLAINED IN A LITTLE MORE DETAIL…
High glucose levels readily cross the placenta and expose the baby to sugars in the Diabetes range, causing complications for the baby.

18+ MILLION WOMEN ARE DIAGNOSED WITH GESTATIONAL DIABETES EVERY YEAR
GESTATIONAL DIABETES OCCURS IN 1 IN 5 PREGNANCIES
The International Diabetes Federation estimated in 2017:
- 204 million women aged 20-79yrs old have diabetes. This number is set to increase to 308 million by 2045
- 1 in 3 women of reproductive age lives with diabetes
- 3 million (16.2%) of live births had some form of hyperglycemia in pregnancy. It was estimated that 85.1% were directly due to Gestational Diabetes
- 1 in 7 births was affected by Gestational Diabetes
- Hyperglycemia in pregnancy is most prominent in low- and middle-income countries where maternal care is limited
What are the risk factors for developing Gestational Diabetes?
We hate to alarm everyone, but all pregnant women are at risk of developing Gestational Diabetes, so it is recommended that all pregnant women are screened using a glucose tolerance blood test at 24-28 weeks’ gestation.
Some women are at a much higher risk and should be screened before becoming pregnant at 12 weeks’ gestation and again at 24-28 weeks if not previously diagnosed.
Several risk factors increase your likelihood of developing Gestational Diabetes. Like with Type 2 Diabetes, extra weight is linked to Gestational Diabetes. This means women who are overweight or obese may already have insulin resistance before they become pregnant. Gaining too much weight during pregnancy can also increase the risk of developing Gestational Diabetes.

Other high-risk factors for developing gestational diabetes include:
- Women aged 25 years or over
- A family history of Type 2 Diabetes (mother or father)
- A family history of Gestational Diabetes, especially from a first-degree relative like a mother or sister
- Being overweight, obese, or morbidly obese
- Had Gestational Diabetes in a previous pregnancy
- Multiple pregnancies in the past
- Previously gave birth to a large baby (weighing more than 8pds)
- Gained weight rapidly during the first trimester of pregnancy
- A previous diagnosis of Polycystic Ovary Syndrome
- Are of non-Caucasian descent, including African-American, Aboriginal or Torres Strait Islander, Melanesian, Polynesian, Chinese, Southeast Asian, Middle Eastern or Indian background
Screening for gestational diabetes
How do doctors know when to test for Gestational Diabetes?
How do you test for Gestational Diabetes?
All women should be tested for Gestational diabetes at weeks 24-28 gestation, which is during the second trimester. If a woman is at a high risk of Gestational Diabetes, such as being overweight at the beginning of your pregnancy; have previously had gestational diabetes; or a close family member (i.e., mother, father, or sibling) has diabetes, your doctor is likely to screen you earlier for gestational diabetes.
A pregnancy oral glucose tolerance test involves:
- Fasting overnight (for at least 8 hours)
- An initial blood test to test fasting glucose levels
- Drinking a syrupy glucose solution containing 75 grams of glucose
- Have a blood glucose test at 1 hour after drinking the glucose solution
- Have a final blood glucose test 2 hours after drinking the glucose solution
The diagnosis of Gestational Diabetes is confirmed on high sugar readings at any of the following time points:
- Fasting glucose value
- 1-hour glucose value
- 2-hour glucose value
What are the diagnostic criteria for Gestational Diabetes?
An elevation in blood glucose levels is diagnostic at either the fasting, 1 hour, or 2-hour test. You only need one test to show abnormal blood glucose readings higher than normal values for each time point diagnosed with Gestational Diabetes. JUST ONE TEST!
What are the glycaemic targets in Gestational Diabetes?
There have been no studies that have defined the optimal glycemic targets for ALL women with Gestational Diabetes. Further research is required to determine optimal blood glucose targets; we will work with you to find what works best for you.
Below are suggested target numbers for women with Gestational Diabetes:
- Fasting blood glucose: 5.0mmol/L (90mg/dL) or less
- 1-hour after eating a meal: 7.4mmol/L (134mg/dL) or less
- 2-hours after eating a meal: 6.7mmol/L (120mg/dL) or less
Your specific blood glucose targets may be set by your doctor if you have Type 1 Diabetes but generally, as close to these values is crucial to reduce complications from Gestational Diabetes on the mother and baby.
What are the complications associated with Gestational Diabetes?
Gestational Diabetes is associated with both short-term complications and long-term complications to both the mother and child. It is vital to maintain blood glucose levels as near normal as possible throughout the pregnancy to minimize complications. Safely controlling sugars minimizes the chance of complications from happening.
It is important to remember that Gestational Diabetes complications are different from the complications of type 2 diabetes.
How does Gestational Diabetes affect the mother?
Gestational Diabetes can increase the risk of developing the following complications in the mother:
- Difficult delivery. In Gestational Diabetes, the baby is more likely to be a large baby due to excessive weight. This can result in having a cesarean section or a forceps delivery, which may distress those mothers who wanted to have a natural birth.
- High blood pressure and preeclampsia. Gestational Diabetes increases the risk of high blood pressure, as well as a condition called preeclampsia. Preeclampsia is a dangerous condition that refers to the onset of high blood pressure and evidence of organ dysfunction occurring in the later stages of pregnancy (after 20 weeks gestation). It can lead to severe life-threatening seizures. The organs affected include the kidneys, liver, lungs, and brain. Preeclampsia can also occur for the first-time during delivery. Preeclampsia can be life-threatening to both mother and baby.
- Future Type 2 Diabetes or Gestational Diabetes is likely. In women who have had Gestational Diabetes are at an increased risk of developing Gestational Diabetes again for any future pregnancies. You are also more likely to develop Type 2 Diabetes as you get older. Healthy lifestyle choices help to minimize the risk of Gestational Diabetes and Type 2 Diabetes. Leading a healthy lifestyle following pregnancy reduces the development of Type 2 Diabetes by 50% or more.
HIGH BLOOD SUGAR IN PREGNANCY PUTS A BABY AT RISK OF DEVELOPING TYPE 2 DIABETES LATER IN LIFE AND BEING OVERWEIGHT EVEN IN THEIR TEENS
How does Gestational Diabetes affect the baby?
Some complications the baby may experience include being bigger at birth with the associated risks of delivering a large baby. Babies are also more immature and can experience breathing difficulties after birth and deficient blood sugar levels. In the long term, a child exposed to high blood sugar levels during gestation is more likely to be overweight and develop diabetes once an adult.
Increased birth weight.
Excessive birth weight, also referred to as large for gestational age, occurs due to increased glucose in your bloodstream crossing the placenta. This causes your baby’s pancreas to start producing extra insulin, resulting in the baby growing too large. Huge babies, weighing 9 pounds or more, can become stuck in the birth canal, causing injuries to you or require an emergency C-section.
Early birth and respiratory distress syndrome.
High blood glucose levels may increase the risk of a mother experiencing early labor and delivering the baby before the due date. Babies that are born too early may experience respiratory distress syndrome, which is a condition that makes breathing difficult and requires assistance breathing. Babies born to mothers with Gestational Diabetes could experience respiratory distress syndrome without being born early
Hypoglycemia
(low blood glucose). Babies of mothers with gestational diabetes may experience low blood glucose levels shortly after birth if their own insulin production is too high.
Type 2 Diabetes later in life.
Babies are at an increased risk of developing Type 2 Diabetes later in life if their mother had Gestational Diabetes
How is Gestational Diabetes treated?
If you have Gestational Diabetes, it is important to regularly monitor and control your blood glucose levels to keep you and your baby healthy. This is important, as it can help you avoid any complications for you and your baby during pregnancy and delivery and later in life.
Lifestyle management
The preferred method of managing gestational diabetes is through lifestyle management, such as diet and exercise. Some women may be required to take medications in pregnancy, for example, metformin or insulin. Metformin is a common drug recommended for Gestational Diabetes, which studies have shown to be safe for use in pregnancy. 30-50% of women with Gestational Diabetes will likely require short term insulin to achieve excellent and safe sugar levels.
Healthy diet
Any recommended diet changes are based on optimal nutrition for the mother and infant and controlled weight gain. Like with a Type 2 Diabetes diet, eating the right food types during pregnancy can help control your blood glucose levels and avoid excess weight gain.
A mother needs to eat enough carbohydrates to prevent ketones from developing but not too much to put too much glucose into the circulation.
Women with Gestational Diabetes need to eat a balanced diet that contains nutrients from all food groups. It is best to completely avoid a keto diet as this may be seriously harmful to the baby. The best diet involves eating a little of everything but not too much.
Exercise
Regular physical activity plays a key role before, during, and after pregnancy. Exercise is very beneficial in aiding with controlled weight. Exercise can lower blood glucose levels by increasing your cells’ sensitivity to insulin. This means your body needs to produce less insulin to transport glucose from the bloodstream and into your cells.

Blood glucose monitoring
Your doctor or endocrinologist may ask you to check your blood glucose levels regularly throughout the day, including when you first wake up in the morning fasting and after you eat your meals at either 1 hour or 2 hours after eating. This is to make sure that your blood glucose levels are staying in a safe range. We have Diabetes Specialists available to review your numbers 24/7.
You can test your blood glucose levels with a blood glucose meter by placing a drop of blood on a test strip. You can use a lancet (a small needle) to produce a drop of blood. Once the blood is applied to the test strip, it is inserted into the blood glucose meter, displaying your blood glucose reading. We have supplies on hand at our clinic.
Does Gestational Diabetes go away after delivery?
Generally, most cases of Gestational Diabetes disappear after pregnancy. However, we will need to confirm 6-10 weeks after delivery with another 2-hour glucose tolerance test.
50% of mothers with Gestational Diabetes will develop Type 2 Diabetes later in life, which is more likely if the correct lifestyle changes are not undertaken. Type 2 Diabetes may develop immediately after the pregnancy or many years later.
Mothers with Gestational Diabetes should have yearly or 2nd yearly screening for Type 2 Diabetes for the rest of their life. If a mother with previous Gestational, Diabetes becomes pregnant again, then the next pregnancy should always be considered high risk for subsequent diabetes and be tested early in pregnancy.


Can Gestational Diabetes be prevented?
Gestational Diabetes is more likely to occur if a person has certain risk factors, but it can also occur without any identifiable risk. Risk factors are either fixed and cannot be changed, called non-modifiable risk factors, such as your ethnicity, age, or family history.
There are some risk factors, modifiable risk factors, that can be changed. These include your weight, diet, and the amount you exercise. When planning for pregnancy, adjusting these modifiable risk factors is a great place to start to help reduce your risk of developing Gestational Diabetes. Some changes are around diet and weight management and are part of preparing for pregnancy. If you have previously had Gestational Diabetes, there are key steps you can take to reduce your risk of Gestational Diabetes. These are all covered in our Direct Diabetes Care™ plans.
What should I do next?
If you experience any symptoms of Gestational Diabetes or you have risk factors for developing Gestational Diabetes, it is important to be tested at 24-28 weeks gestation. Some people are at higher risk than others. If you are 25 years or older or have other risk factors for diabetes, you may require testing earlier in pregnancy. By diagnosing and treating Gestational Diabetes, it means you can decrease the risk of developing or delay any further health complications of Gestational Diabetes. These complications can affect both you and your child later in life; for example, you are both at risk of developing Type 2 Diabetes. It is important to know that diagnosing diabetes should not rely solely on using a Hb A1c test.

Once we learn what your diagnosis is, or if you already have Gestational or Type 2 Diabetes, the next most important step is to become educated. We work along with your OB-GYN throughout your interior pregnancy plus test you after delivery. By joining the DiabetesDirectCare™ program, you will receive the help and education you need to learn how best to manage your condition. For example, you will learn how best to monitor blood glucose levels and review different diabetic supply options. The DDC program is personalized and tailored, giving you more of the content you want when you want it. With 24/7 care 365 days a year, you have Diabetes Specialists ready to help you when you need it most. The DDC program also keeps you motivated and teaches you what changes you need to make.
From your first appointment, the DDC program is full of helpful and crucial information.
Gestational Diabetes Resources
