Beyond BMI: Rethinking Obesity Assessment for Better Health Outcomes
The Body Mass Index (BMI) has long been the go-to measure for assessing weight categories and associated health risks. However, recent research suggests that relying solely on BMI may not provide an accurate picture of obesity. To address this concern, researchers have explored alternative measures to improve the assessment of body fat percentage and overall health. In this blog post, we delve into the limitations of BMI, highlight a recent study’s findings, and discuss the importance of incorporating additional measures to obtain a comprehensive understanding of obesity and its associated risks.
The Limitations of BMI:

BMI is calculated by dividing an individual’s weight by the square of their height and has been widely used to categorize weight status. However, it fails to consider factors such as fat distribution, muscle mass, bone density, and racial and sexual differences. These limitations have raised questions about its effectiveness as a sole measure for determining obesity and related health risks.
New Study Highlights BMI’s Inadequacy
A recent study presented at the Endocrine Society’s annual meeting shed light on the shortcomings of BMI in predicting obesity. The researchers analyzed data from nearly 10,000 participants, comparing BMI classifications with measurements of body fat percentage using dual-energy X-ray absorptiometry (DEXA).
Surprisingly, the study revealed that BMI predicted less than half of the participants with obesity as indicated by body fat percentage. While only 36% of participants were classified as obese by BMI, close to 74% fell into the obese category when considering body fat percentage. This disparity underscores the need for supplementary measures to accurately assess weight and overall health.
Additional Factors That Should Be Considered In Obesity Assessment
To obtain a comprehensive understanding of obesity and its associated risks, healthcare professionals should consider several alternative measures alongside BMI. These measures include:
Visceral Fat Measurements:
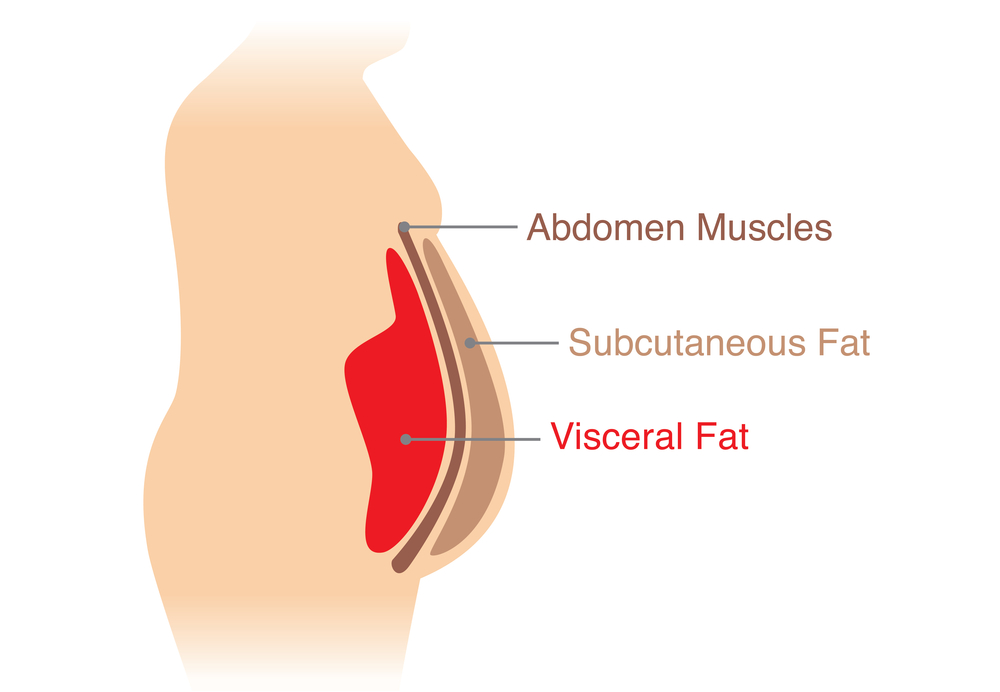
Assessing visceral fat, which accumulates around the abdomen, provides valuable insights into obesity-related health risks. Imaging techniques such as MRI or CT scans can help evaluate the amount of visceral fat present.
Body Adiposity Index (BAI):
BAI takes into account hip circumference and height to estimate body fat percentage. By incorporating BAI, healthcare professionals can obtain a more accurate assessment of adiposity.
Body Composition Analysis:

Dual-energy X-ray absorptiometry (DEXA) scans or bioelectrical impedance analysis allow for a detailed breakdown of body composition, including muscle mass, bone density, and body fat percentage. This analysis offers valuable insights into an individual’s overall health and risk of obesity-related complications.
Genetic and Lifestyle Factors:
Considering genetic and metabolic factors can provide additional information about an individual’s predisposition to obesity and associated health risks. These factors help tailor interventions and preventive strategies to address specific needs.

Basal Metabolic Rate (BMR):
Calculating BMR provides insights into the minimum caloric intake required for basic bodily functions. Understanding an individual’s BMR aids in developing personalized nutrition plans that support weight management and overall health.
Conclusion
While BMI has been a widely used measure for assessing weight categories, its limitations in predicting obesity and related health risks are becoming increasingly apparent. Incorporating alternative measures such as visceral fat measurements, body adiposity index, body composition analysis, genetic and lifestyle factors, and basal metabolic rate can offer a more comprehensive understanding of an individual’s health status. By embracing a more holistic approach to obesity assessment, healthcare professionals can tailor interventions and preventive strategies to promote better health outcomes for all individuals, irrespective of their BMI classification.

Other recent articles that have been posted about BMI:
https://www.nbcnews.com/health/health-news/overreliance-bmi-can-stand-patients-treatment-rcna51228
https://www.goodmorningamerica.com/wellness/video/ama-asks-doctors-de-emphasize-bmi-100063640


